Blog
Common Foot Treatments That Make Your Stay Active
Foot problems can make it harder for us to stay involved in the activities we enjoy. Whether it’s a mild ache that gets worse with time or a sudden injury that slows us down, foot problems tend to affect everything ...
Continue Reading →
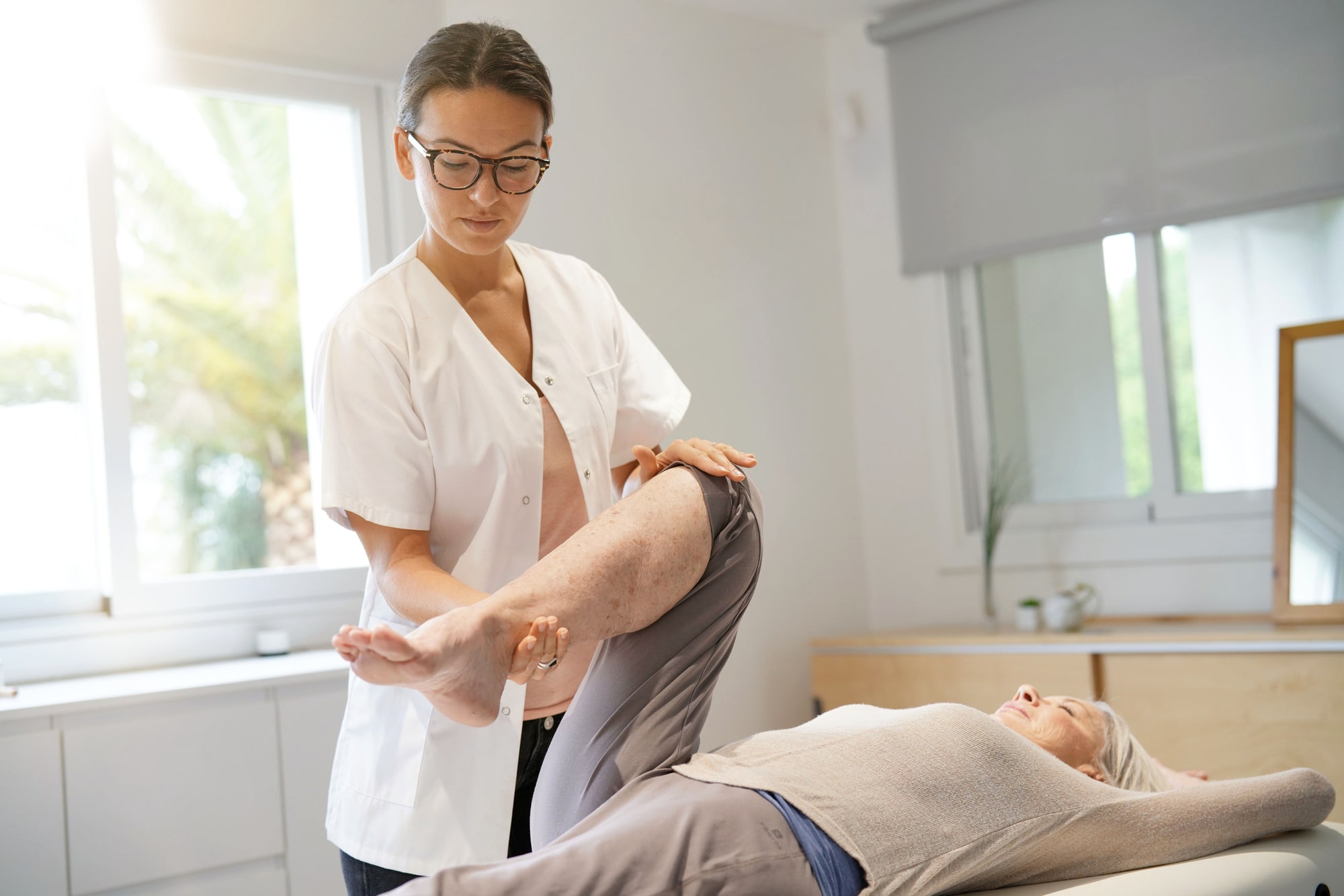
How An Orthopedic Rehabilitation Program Works
Recovering from an injury or surgery often requires a structured approach to regain strength, mobility, and function. Orthopedic rehabilitation focuses on helping individuals recover from musculoskeletal conditions, including joint injuries, fractures, and post-surgical recovery. Knowing what to expect during the ...
Continue Reading →
How Slips And Falls Can Lead To Serious Foot Injuries
We’ve seen firsthand how slip-and-fall accidents can leave individuals dealing with serious foot injuries that disrupt daily life. Our friends at Cohen & Cohen discuss how such accidents not only cause pain and mobility challenges but can also lead to ...
Continue Reading →
Podiatry Gift Ideas for Health-Conscious Loved Ones
Podiatry Gift Ideas for Health-Conscious Loved Ones Finding the perfect gift can be challenging, but if you’re shopping for someone who values foot health, podiatry-related gifts are thoughtful and practical. From supportive footwear to pampering products, there are options for ...
Continue Reading →
Foot Health During Pregnancy: What to Expect and How to Care for Your Feet
Pregnancy brings many changes to a woman’s body, and while the focus is often on the growing belly and hormonal shifts, your feet also undergo significant changes. As your body adjusts to accommodate your growing baby, the added weight, hormonal ...
Continue Reading →
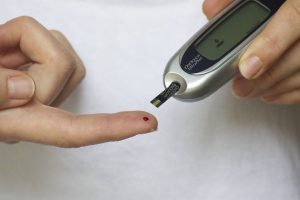
Diabetes and Your Feet: What You Should Know
You may know that diabetes is a chronic disease affecting blood sugar (glucose) and insulin, but did you know that affects approximately 29.1 million people in the United States, which is more than 9% of the population? Every year 1.7 ...
Continue Reading →
Halloween Shoe Safety: How to Protect Your Feet While Enjoying the Festivities
Halloween is one of the most exciting times of the year, filled with costumes, parties, and trick-or-treating adventures. However, while you’re focusing on creating the perfect costume, it’s easy to overlook one of the most important aspects of a fun ...
Continue Reading →
Understanding Sever Disease (Calcaneal Apophysitis): Causes, Symptoms, and Treatment Options
Understanding Sever Disease (Calcaneal Apophysitis): Causes, Symptoms, and Treatment Options Sever disease, also known as calcaneal apophysitis, is a common but often misunderstood condition that affects growing children, particularly those who are physically active. This overuse injury causes pain in ...
Continue Reading →
Choosing Proper Footwear: Steps to Healthy Feet
Selecting the right footwear is not just about fashion; it plays a crucial role in maintaining overall foot health and preventing various foot-related issues. At Dynamic Foot and Ankle Center we understand the importance of proper footwear and its impact ...
Continue Reading →